Last updated on March 26th, 2026 at 12:52 pm
Last updated on November 13th, 2025 at 06:43 pm
How many patients have you lost since opening your practice?
Dentistry has this wonderful advantage built into it where patients know they’re supposed to come back every six months for the rest of their lives. Any other business owner would give their right arm for that!
And yet, just about every time I meet with a dentist for the first time I find that they’ve been driving themselves crazy trying to get new patients—and are shocked when we do the calculations to discover how many patients of record they’ve lost over the years.
In most cases, the answer to increasing production and income usually lies first and foremost with retaining the patients you already have, and reactivating those that haven’t been coming in.
Patient retention rate is defined as: the percentage of patients that stay with your practice and continue to keep appointments over time. Obviously, this ties in most with recall appointments and patient compliance with their hygiene appointments, but there are many other factors that impact patient retention.
So, in this post, I want to discuss the most prominent reasons patients don’t come back and the keys to “sealing the leaks” in your practice by improving patient retention.
And to calculate your patient loss over time, watch the video Active Vs Total Patient Count: Is Your Practice Growing?
First, the most common reasons patients don’t come back:
1. The patient didn’t schedule their next appointment before leaving the office
 It’s more or less an accepted fact that patients should schedule their next hygiene visit before leaving, and yet in many practices, an unfortunately high number of patients roll through without making an appointment. Fixing this starts with ensuring your entire team understands that this should never happen, along with why.
It’s more or less an accepted fact that patients should schedule their next hygiene visit before leaving, and yet in many practices, an unfortunately high number of patients roll through without making an appointment. Fixing this starts with ensuring your entire team understands that this should never happen, along with why.
Additionally, you should have one person responsible for this. If “everyone” is supposed to be responsible—who’s responsible, then? When it breaks down, the finger-pointing starts—“I thought Jean was supposed to schedule Mr. Smith,” and so on. Put one person in charge of scheduling (i.e. a Schedule Coordinator) and part of their job description should include that every patient is scheduled before leaving. Even if the hygienist schedules a patient in the back, the Scheduling Coordinator would still double-check that a) it was done and b) it was done correctly, and if not—fix it!
2. It’s too hard to schedule an appointment because you’re booked out too far
Many dentists mistakenly think that it’s a good thing to be booked out completely months in advance.
But it’ll actually cause you to a) miss out on potential new patients (which should be gotten in within 24-72 hours ideally), and b) lose existing patients that can’t conform to your schedule.
What if a patient unexpectedly calls in? What if you’re trying to reactivate an overdue patient? What if a patient needs to move their appointment?
If you’ve only got three little openings for that month and the patient can’t come in on those days—they either forget about it next month, give up or go elsewhere.
So if you’re booked up completely months in advance, you may actually be able to significantly increase production and have more flexibility by adding an associate and/or another hygienist.
3. Poor customer service
 Besides the scheduling aspect, retention really comes down to customer service and the patient experience in your office. The patient doesn’t want to feel like they’re just a dollar symbol walking through your business. You need a personal touch.
Besides the scheduling aspect, retention really comes down to customer service and the patient experience in your office. The patient doesn’t want to feel like they’re just a dollar symbol walking through your business. You need a personal touch.
I recommend looking at this article on customer service and taking it to heart, but here are a few key points:
- Staff seeming disinterested, annoyed, or outright rude. Your patients should always be greeted with a smile and shown that you’re happy they are there. If the staff are “too busy,” answering the phone gruffly and putting them on hold, etc., it’ll kill your retention.
- Errors with billing and insurance. Nothing upsets a patient quicker than billing errors or financial misunderstandings.
- Having to wait long amounts of time. I know waiting is common in the medical field, but this shouldn’t happen in your office because it’s a huge turn-off and makes people not want to go to the dentist.
- Failing to answer messages or return phone calls. In fact, I would even recommend having an after-hours answering service if you can, so you receive all patients’ communication and can handle it quickly.
And get creative with adding a personal touch. Pre-op and post-op phone calls to check in on the patient can go a long way. A number of our clients have the doctor or hygienist personally call each new patient on the schedule the day before to introduce themselves, answer any questions, and let them know they are excited to see them tomorrow.
4. A sloppy or uncodified perio protocol
If you don’t have office policy (written by the doctor of course) on perio protocol, you’re potentially creating a number of problems in the practice. Not least of which, you could end up not properly addressing perio issues with patients, and/or doing procedures that you’re not charging for (e.g. classifying what should be a gross debridement as a prophy).
As a result, your patient’s oral health and education may suffer. Instead of knowing they have a perio issue (that required more extensive treatment), and improving home care, they instead may think everything’s “OK,” and continue business as usual.
This is really one of these win-win scenarios—your patient’s health and potentially office productivity (when more extensive treatment is warranted), both can see improvement.
5. Rushing through case presentations and/or focusing too much on insurance or discounts.
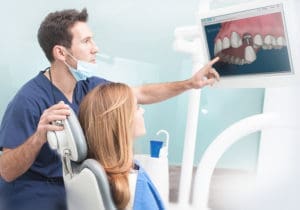 Here’s a common scenario: The doctor only has a couple minutes, so they quickly tell the patient what they need and send them up front. Then the patient sees the price… their eyes bulge…and then they leave without scheduling. They are going to “think about it.” They don’t really understand why they need it, but they do understand the finances involved. They end up on the incomplete treatment list and in some cases, going elsewhere for a second opinion.
Here’s a common scenario: The doctor only has a couple minutes, so they quickly tell the patient what they need and send them up front. Then the patient sees the price… their eyes bulge…and then they leave without scheduling. They are going to “think about it.” They don’t really understand why they need it, but they do understand the finances involved. They end up on the incomplete treatment list and in some cases, going elsewhere for a second opinion.
So don’t scare a patient off with a rushed case presentation. Make sure you have enough time to properly present treatment and ensure your patient truly understands, along with answering any questions they have.
If you don’t have time for that now, schedule them to come back in for a consult.
Here’s another common scenario: A doctor (or the Financial Coordinator) tells a patient the cost for a crown is $1200. Patient says they can’t afford it, so the price is immediately dropped by $300. Obviously, not a good idea! And believe it or not, this happens more than you might think.
Beyond this being bad business, what does that tell a patient? It tells them you must have been trying to price gouge them before you agreed to give them a discount! It devalues your service.
So, assuming your fees are fair—charge that fee! If you want to see what fees are in your area by procedures, you can always consult the Wasserman Guide (https://wasserman-medical.com/shop/product/ndas-medical-dental-coding-fee-guide-2020-9th-edition/). I’d recommend you don’t go below the 60th percentile. Ultimately though the decision on how you want to do this is up to you. Our COO, Jeff Blumberg wrote an article and did a video on the subject of fees as well.
If you’re struggling with case acceptance, we can help with the MGE Communication & Sales Seminars.
And here’s one last common scenario: Patient only does the one or two crowns that insurance will cover, even though they really needed six crowns. In their mind, they saved money and maximized their insurance. They are healthier—but not completely. Their oral health is still compromised.
Your practice exists to help people restore and maintain their oral health. And with your skills, you can do some pretty incredible life-changing things. When you get that result, patients love you for it. But if you don’t, and you’re only doing single-tooth dentistry and partial treatment plans, patients never experience that fantastic result that creates loyalty to your practice.
Case acceptance is a huge part of patient retention. It’s a lot bigger than you might think. And it shouldn’t be overlooked.
6. Retiring charts too quickly and/or not following up enough with overdue patients
There are only four circumstances in which you would “purge” or deactivate a chart:
- The doctor doesn’t want this patient in the practice anymore
- The patient moved away, (out of state, etc.) and they’ve told you they won’t be coming back,
- The patient has left the practice,
- The patient has passed away

In all other scenarios, don’t retire the chart. Work to reactivate them!
I don’t care if it’s been five years or even ten since you saw them last. If they haven’t requested their records, then most likely they still consider you to be their dentist. Time just slipped by and they didn’t realize how long it’s been.
At MGE, we provide our clients with a step-by-step reactivation program to get these overdue patients back in the chair, and it works wonders! If you do it consistently, you will get patients back in the chair and build up your Hygiene Department. You can also find more information on the subject in these articles.
For in-depth training on reactivation, I’d recommend you check out our on-demand video training platform, DDS Success (free demo).
We recommend taking your whole list of unscheduled and overdue patients (not just “active” patients, but ALL patients) and going through that whole list to reach out to them. You call each one and follow that up with a text message or email and a letter.
And then when you get to the end, go back to the beginning and start again. It’s an ongoing action.
We find that statistically, it may take up to 12 attempts over time—i.e. email, text, phone, etc… to reach someone in order to get them back in. So if you only follow up once or twice, you’re going to miss out on the vast majority of your overdue patients.
Have your team dedicate time to this on a weekly basis.
7. Patients don’t understand the importance of recall visits and maintenance
As we mentioned above under point “4,” it’s critical that your patients understand the importance of regular hygiene visits. And a key part of your hygienist’s job description is being an educator for your patients. The doctor and assistants should also reinforce this with patients.
And this is the main reason we’re not huge fans of assisted (accelerated) hygiene. Going through the hygiene appointments so fast means the hygienist doesn’t have enough time to build the relationship and educate the patient, and the doctor doesn’t have enough time for case acceptance.
SUMMARY: Steps to “seal the leak” and improve patient retention
Taking into account all the points mentioned above, here are a few steps you could take now:
- Take a look at your scheduling methodology to see how you can ensure you don’t miss anyone, run on-time, and make it easier to get patients in quickly.
- Get together with your team to go over customer service. We can help you with this with our online Customer Service Course on DDS Success. Look at the patient flow and isolate anything in the practice that may lower the quality of customer service—and then work as a team to fix these points.
- Create Perio Protocol policies for your practice. And then meet with your hygienist(s) to answer any questions so you’re all on the same page.
- Improve your case acceptance skills. There are a lot of resources for you to improve your case presentations and teach your staff how to handle financial arrangements. You can start with our on-demand video courses on DDS Success, and you can attend the MGE Communication & Sales Seminars—which can now be live-streamed online so you can attend from home.
- Implement a reactivation program and keep it going on a continual basis. There are always patients to reactivate, so always be going through that list and getting patients back in the chair.
- Focus on educating your patients about hygiene and reinforce it each time they come in.
Hope this helps!
And if you need any help at all or have more questions, you can reach us any time at (800) 640-1140 or schedule a free consultation.


No Comments
Be the first to start a conversation